Connect With Us

Recognizing the Symptoms of Flat Feet

Flat feet, or fallen arches, are a common condition where the arches of the feet collapse, causing the entire sole to touch the ground. Recognizing the symptoms of flat feet is essential for understanding and addressing this condition. One prevalent sign is pain or discomfort along the inner side of the ankle and arch. Individuals with flat feet may also experience swelling along the inside of the ankle. The lack of a visible arch when standing or walking is a visual indicator of flat feet. Overpronation, where the foot rolls inward excessively, can contribute to this condition and lead to related issues, including shin splints or knee pain. Fatigue and aching in the feet and legs can occur, especially after prolonged standing. If you have flat feet, it is suggested that you speak to a podiatrist who can provide you with effective relief options.
Flatfoot is a condition many people suffer from. If you have flat feet, contact Charles Passet, DPM from Forest Hills. Our doctor will treat your foot and ankle needs.
What Are Flat Feet?
Flatfoot is a condition in which the arch of the foot is depressed and the sole of the foot is almost completely in contact with the ground. About 20-30% of the population generally has flat feet because their arches never formed during growth.
Conditions & Problems:
Having flat feet makes it difficult to run or walk because of the stress placed on the ankles.
Alignment – The general alignment of your legs can be disrupted, because the ankles move inward which can cause major discomfort.
Knees – If you have complications with your knees, flat feet can be a contributor to arthritis in that area.
Symptoms
- Pain around the heel or arch area
- Trouble standing on the tip toe
- Swelling around the inside of the ankle
- Flat look to one or both feet
- Having your shoes feel uneven when worn
Treatment
If you are experiencing pain and stress on the foot you may weaken the posterior tibial tendon, which runs around the inside of the ankle.
If you have any questions please feel free to contact our office located in Forest Hills, NY . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
What is Flexible Flat Foot?
Flatfoot is classified as having the entire sole of the foot in contact or near contact to the ground while standing. The disorder is also known as fallen arches, because those affected have no arch in their feet. Flexible flatfoot and rigid flatfoot are the two types of flatfoot.
A person has flexible flatfoot if when sitting or standing on their toes, they have an arch that disappears when they stand with the entire foot on the ground. Flexible flatfoot may also be called “pediatric flatfoot” because the condition first appears in childhood. It is common among infants because the arch does not develop until the age of 5 or 6 years. Rigid flatfoot is not as common in children as it is with adults. This type of flatfoot is developed due to the weakening of tibialis posterior muscle tendon, a major supporting structure of the foot arch. Development of this deformity is progressive and shows early signs of pain and swelling that begins at the inside arch of the foot and moves to the outside of the foot below the ankle. More severe cases can possibly lead to arthritis of the foot and ankle joints.
Although most cases of flatfoot involve people born with the condition, some less common causes are obesity, diabetes, pregnancy, and osteoporosis. In some cases, flatfoot may come with no symptoms at all and does not require any type of treatment. With other cases though, symptoms may include pain in the shin, knee, hips and lower back. If a person with flatfeet experiences such symptoms, a health care provider may suggest using orthotic devices or arch supports, which may reduce the pain. Wearing supportive shoes can also prove more comfortable with flatfeet and staying away from shoes with little support such as sandals. Other methods to relieve pain also include stretching the Achilles tendon properly and using proper form when doing any physical activity. In addition, losing weight can reduce the stress on your feet and reduce the pain.
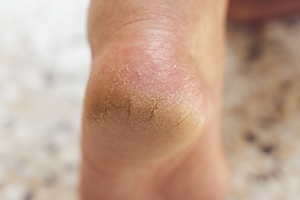
Common Reasons Why Cracked Heels Develop

Cracked heels, also known as heel fissures, are a common foot ailment that can be both unsightly and uncomfortable. Several factors contribute to their development. One primary cause is dry skin. The skin on the soles of your feet is naturally thicker, and when it lacks moisture, it becomes less flexible and more prone to cracking. Another factor is inadequate hydration. Dehydration can affect your body's ability to maintain skin elasticity, making it easier for your heels to crack. Additionally, prolonged standing, especially on hard surfaces, can also contribute to this problem, as it puts extra pressure on the heel area and may lead to cracks. Footwear choices play a significant role. Wearing open-back or poorly fitting shoes can increase friction and pressure on the heel, exacerbating the issue. Various medical conditions, such as diabetes or thyroid disorders, can also affect skin health and potentially lead to cracked heels. People may have lifestyle factors such as excessive bathing or exposure to harsh, dry climates which can contribute to developing cracked heels. If you have cracked heels, it is strongly suggested that you visit a podiatrist who can offer you effective treatment options, which may include prescribed medication.
If the skin on your feet starts to crack, you may want to see a podiatrist to find treatment. If you have any concerns, contact Charles Passet, DPM from Forest Hills. Our doctor can provide the care you need to keep you pain-free and on your feet.
Cracked Heels
It is important to moisturize your cracked heels in order to prevent pain, bleeding, and infection. The reason cracked heels form is because the skin on the foot is too dry to support the immense pressure placed on them. When the foot expands, the dry skin on the foot begins to split.
Ways to Help Heal Them
- Invest in a good foot cream
- Try Using Petroleum Jelly
- Ease up on Soaps
- Drink Plenty of Water
Ways to Prevent Cracked Heels
- Moisturize After Showering
- Skip a Shower
- Keep Shower Water Lukewarm
- Don’t Scrub Your Feet
If you are unsure how to proceed in treating cracked heels, seek guidance from a podiatrist. Your doctor will help you with any questions or information you may need.
If you have any questions, please feel free to contact our office located in Forest Hills, NY . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Solutions for Cracked Heels
Cracked heels may make you want to think twice about showing off your feet in warmer weather. However, cracked heels may be harmful to more than just the appearance of your feet. If deep fissures and cracks develop in your heels, they may make walking and standing painful for you. Additionally, these openings make way for germs to enter through your skin and cause infection.
There are several different causes of cracked heels. One of the most common reasons for this ailment is dry skin. This problem may make your keeps feel rough tight and itchy. Dry skin may be caused by cold air, extremely hot water, harsh soaps, and aging. Skin disorders such as eczema and psoriasis may eventually lead to dry skin. In some cases, complications may arise from cracked heels. Some of these complications are a loss of feeling in the heel, cellulitis, or a diabetic foot ulcer.
There are ways you can try to prevent getting cracked heels. One of the best ways to do so is to avoid wearing flip flops and sandals because these shoes increase your risk of drying out your feet. You should also avoid wearing shoes with a tall skinny heel, because these shoes cause your heel to expand sideways. At night, you should slather on a thick moisturizing cream on your feet and then cover them in socks to keep your feet moisturized overnight. Drinking water to stay hydrated is also a good way to ensure that your skin doesn’t become dry.
If you suffer from a severe case of cracked feet, you should make an appointment with your podiatrist to see what treatment methods are best for you.
Are Bunions Affecting Your Everyday Life?
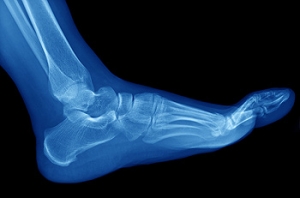
Causes and Symptoms of Foot Stress Fractures

Stress fractures, those tiny cracks in the bones of the feet, are a common concern for athletes, dancers, and anyone who spends a significant amount of time on their feet. These fractures are usually a result of repetitive stress and overuse, rather than sudden trauma. One primary cause of stress fractures is overexertion, often seen in athletes who increase their training intensity too quickly. Wearing Improper footwear or a sudden change in physical activity can also put undue stress on the bones. Inadequate nutrition and underlying conditions such as osteoporosis may weaken bones, making them more susceptible to fractures. Symptoms of a stress fracture typically include localized pain, swelling, and tenderness in the affected area. The pain usually worsens with activity and eases with rest. Left untreated, stress fractures can progress to chronic pain and complications, so early intervention is essential. Understanding the causes and recognizing these symptoms allows for prompt diagnosis and proper care, reducing the risk of more severe injuries and ensuring a quicker return to an active, pain-free lifestyle. If you have developed a foot stress fracture, it is suggested that you visit a podiatrist as quickly as possible who can effectively treat this condition.
Stress fractures occur when there is a tiny crack within a bone. To learn more, contact Charles Passet, DPM from Forest Hills. Our doctor can provide the care you need to keep you pain free and on your feet.
How Are They Caused?
Stress fractures are the result of repetitive force being placed on the bone. Since the lower leg and feet often carry most of the body’s weight, stress fractures are likely to occur in these areas. If you rush into a new exercise, you are more likely to develop a stress fracture since you are starting too much, too soon. Pain resulting from stress fractures may go unnoticed at first, however it may start to worsen over time.
Risk Factors
- Gender – They are more commonly found in women compared to men.
- Foot Problems – People with unusual arches in their feet are more likely to develop stress fractures.
- Certain Sports – Dancers, gymnasts, tennis players, runners, and basketball players are more likely to develop stress fractures.
- Lack of Nutrients – A lack of vitamin D and calcium may weaken the bones and make you more prone to stress fractures
- Weak Bones – Osteoporosis can weaken the bones therefore resulting in stress fractures
Stress fractures do not always heal properly, so it is important that you seek help from a podiatrist if you suspect you may have one. Ignoring your stress fracture may cause it to worsen, and you may develop chronic pain as well as additional fractures.
If you have any questions, please feel free to contact our office located in Forest Hills, NY . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Dealing with Stress Fractures of the Foot and Ankle
Stress fractures are small breaks in the bone that are caused by repetitive stress. They typically occur due to overuse, forcing the bones of the foot or ankle to continually absorb the full impact of each step taken. Stress fractures can also be caused by abnormal foot structure, osteoporosis, bone deformities, or wearing improper footwear during exercise.
Stress fractures are common for individuals whose daily activities cause high levels of impact on their feet and ankles. Those who run, play tennis or basketball, or practice gymnastics tend to experience these fractures more frequently. Anyone is susceptible to this problem, though. Individuals who are normally sedentary and suddenly begin an intense, high impact workout may sustain stress fractures. This is because their muscles are not yet strong enough to handle and cushion the intensity of their activity. Osteoporosis may also cause someone to get stress fractures, because the disease weakens an afflicted person's bones and makes it easier for them to break down.
Pain from stress fractures typically occurs in the general area of the fracture. Pain can also manifest as “pinpoint pain” or pain that is felt when the site of the injury is touched, and can be accompanied by swelling. It may occur during or after activity, and it may disappear while resting and return when standing or moving. Engaging in any kind of activity, high impact or otherwise, will aggravate the pain. If the intensity of the activity increases before the stress fracture has properly healed, it can cause a full fracture.
Treatment can vary depending on the individual and the degree of injury. The primary way to treat a stress fracture is to rest the hurt foot. Some fractures will heal quickly with only a little bit of rest, while others may require a long rest period and the use of crutches, immobilization, or physical therapy. Under certain circumstances, surgery may be required to install support pins around the fracture to assist in healing.
If you are undergoing a new exercise regimen in running or some other kind of high impact activity, set incremental goals on a weekly basis so you can build up muscle strength. Make sure to wear supportive shoes to better protect you feet.
If you begin to experience any symptoms of stress fractures, you should stop exercising and rest. If the symptoms persist, consult with your podiatrist. Remembering these tips can help you prevent stress fractures to your foot and ankle, and allow you to continue living normally.
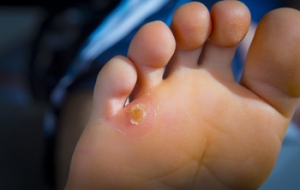
Surgery May Relieve Painful Corns

Corns on the feet are most commonly caused by excessive pressure on the toe or bottom of the foot from wearing tight or ill-fitting shoes. When painful corns on your feet become unbearable and conservative treatments no longer work, surgery is a viable option. Corns, known medically as heloma, can become excruciating, making even the simplest daily activities a painful ordeal. The surgical procedure involves making a small incision over the affected toe to access the corn. The foot doctor removes the corn, repairs any tendon that may be involved, and closes the incision. Various numbing options, including general anesthesia, a spinal block, or local anesthesia with sedation, are offered based on the severity of the procedure. Surgery for painful corns addresses the root causes of discomfort and can provide a permanent solution. If persistent corn-related pain affects your life, it is suggested that you make an appointment with a podiatrist. This foot doctor can assess the need for surgery or offer other treatment options as needed.
Corns can make walking very painful and should be treated immediately. If you have questions regarding your feet and ankles, contact Charles Passet, DPM of Forest Hills. Our doctor will treat your foot and ankle needs.
Corns: What Are They? And How Do You Get Rid of Them?
Corns are thickened areas on the skin that can become painful. They are caused by excessive pressure and friction on the skin. Corns press into the deeper layers of the skin and are usually round in shape.
Ways to Prevent Corns
There are many ways to get rid of painful corns such as:
- Wearing properly fitting shoes that have been measured by a professional
- Wearing shoes that are not sharply pointed or have high heels
- Wearing only shoes that offer support
Treating Corns
Although most corns slowly disappear when the friction or pressure stops, this isn’t always the case. Consult with your podiatrist to determine the best treatment option for your case of corns.
If you have any questions please feel free to contact our office located in Forest Hills, NY . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Corns and Calluses
A corn is a lesion that forms in the skin of the foot, and it is typically circular in shape, small in size, and thick and rough in texture. A corn generally occurs as a result of repeated pressure on the skin; one example of this is the rubbing of a shoe against the skin. Corns differ from calluses in that their central cores are harder in texture.
A corn is a relatively common condition with a wide variety of treatment options. If a corn becomes overly uncomfortable or painful, consult with your podiatrist; he can determine the best method of treatment that is appropriate for you. Corns may return if the underlying cause of its development is not treated or removed. Avoid removing corns at home, as improper removal may cause infection.
A callus, similar to a corn, is an area of skin that has become thickened due to repeated pressure and rubbing. The rubbing causes the skin to create a layer of protective skin, which is the formed callus. Calluses can differ in size between people, and they can also become painful.
Multiple treatments are available for calluses. At-home treatment and removal should be avoided, as this can potentially lead to infection. Your podiatrist can best determine the cause of your calluses and suggest the treatment most appropriate for you.
Need for Vascular Testing With Lower Extremity Issues

Peripheral vascular disease, also known as PVD, is a prevalent issue, especially among diabetics. It affects over five million people each year and contributes to complications such as lower extremity wounds and amputations. Given its widespread incidence, obtaining an accurate diagnosis is critical for effective management and prevention of severe outcomes. There are non-invasive screening methods that podiatrists can incorporate into their initial patient evaluations, and they are deemed highly effective for identifying peripheral arterial diseases, particularly in at-risk populations. If you have PVD or lower extremity issues, it is strongly suggested that you make an appointment with a podiatrist for a comprehensive vascular assessment and treatment.
Vascular testing plays an important part in diagnosing disease like peripheral artery disease. If you have symptoms of peripheral artery disease, or diabetes, consult with Charles Passet, DPM from Forest Hills. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
What Is Vascular Testing?
Vascular testing checks for how well blood circulation is in the veins and arteries. This is most often done to determine and treat a patient for peripheral artery disease (PAD), stroke, and aneurysms. Podiatrists utilize vascular testing when a patient has symptoms of PAD or if they believe they might. If a patient has diabetes, a podiatrist may determine a vascular test to be prudent to check for poor blood circulation.
How Is it Conducted?
Most forms of vascular testing are non-invasive. Podiatrists will first conduct a visual inspection for any wounds, discoloration, and any abnormal signs prior to a vascular test.
The most common tests include:
- Ankle-Brachial Index (ABI) examination
- Doppler examination
- Pedal pulses
These tests are safe, painless, and easy to do. Once finished, the podiatrist can then provide a diagnosis and the best course for treatment.
If you have any questions, please feel free to contact our office located in Forest Hills, NY . We offer the newest diagnostic and treatment technologies for all your foot care needs.